Coronavirus symptoms: 10 keys signs and how to protect yourself
 |
| Shortness of breath is one key sign of COVID-19 (Photo: mypict.org) |
Shortness of breath
Shortness of breath is not usually an early symptom of COVID-19, but it is the most serious. It can occur on its own, without a cough. If your chest becomes tight or you begin to feel as if you cannot breathe deeply enough to fill your lungs with air, that's a sign to actquickly, experts say.
"If there's any shortness of breath immediately call your health care provider, a local urgent care or the emergency department," American Medical Association president Dr. Patrice Harris told CNN in a statement. "If the shortness of breath is severe enough, you should call 911”.
The CDC lists other emergency warning signs for COVID-19 as a "persistent pain or pressure in the chest," and "bluish lips or face," which can indicate a lack of oxygen.
Get medical attention immediately, the CDC says.
Fever
Fever is a key sign of COVID-19. Because some people can have a core body temperature lower or higher than the typical 98.6 degrees Fahrenheit (37 degrees Celsius), experts say not to fixate on a number.
Most children and adults, however, will not be considered feverish until their temperature reaches 100 degrees Fahrenheit (37.7 degrees Celsius).
| Don't rely on a temperature taken in the morning, said infectious disease expert Dr. William Schaffner, a professor of preventative medicine and infectious disease at Vanderbilt University School of Medicine in Nashville. Instead, take your temperature in the late afternoon and early evening. "Our temperature is not the same during the day. If you take it at eight o'clock in the morning, it may be normal," Schaffner explained, adding that "Our temperature is not the same during the day. If you take it at eight o'clock in the morning, it may be normal”. |
Dry Cough
Coughing is another common symptom, but it's not just any cough. The cough is bothersome, a dry cough that you feel deep in your chest.
"It's coming from your breastbone or sternum, and you can tell that your bronchial tubes are inflamed or irritated," Schaffner added.
A report put out by the World Health Organization in February found over 33% of 55,924 people with laboratory confirmed cases of COVID-19 had coughed up sputum, a thick mucus sometimes called phlegm, from their lungs.
Chills and body aches
Not everyone will have such a severe reaction of chills and body aches when they catch the virus, experts say.
Some may have no chills or body aches at all. Others may experience milder flu-like chills, fatigue and achy joints and muscles, which can make it difficult to know if it's flu or coronavirus that's to blame.
One possible sign that you might have COVID-19 is if your symptoms don't improve after a week or so but actually worsen.
Sudden confusion
Speaking of worsening signs, the CDC says a sudden confusion or an inability to wake up and be alert may be a serious sign that emergency care may be needed. If you or a loved one has those symptoms, especially with other critical signs like bluish lips, trouble breathing or chest pain, the CDC says to seek help immediately.
Digestive issues
At first science didn't think diarrhea or other typical gastric issues that often come with the flu applied to the noval coronavirus, also known as SARS-CoV-2. As more research on survivors becomes available, that opinion has changed.
"In a study out of China where they looked at some of the earliest patients, some 200 patients, they found that digestive or stomach GI (gastrointestinal) symptoms were actually there in about half the patients," Gupta said on CNN's New Day news program.
The study described a unique subset of milder cases in which the initial symptoms were digestive issues such as diarrhea, often without fever. Those patients experienced delays in testing and diagnosis than patients with respiratory issues, and they took longer to clear the virus from their systems.
 |
| Pink eye could be one more sign and you should call doctor if you also have other telltale symptoms like fever, cough or shortness of breath (Photo: BI) |
Pink eye
Research from China, South Korea and other parts of the world indicate that about 1% to 3% of people with COVID-19 also had conjunctivitis, commonly known as pink eye.
Conjunctivitis, a highly contagious condition when caused by a virus, is an inflammation of the thin, transparent layer of tissue, called conjunctiva, that covers the white part of the eye and the inside of the eyelid.
But SARS-CoV-2 is just one of many viruses that can cause conjunctivitis, so it came as no real surprise to scientists that this newly discovered virus would do the same.
Still, a pink or red eye could be one more sign that you should call your doctor if you also have other telltale symptoms of COVID-19, such as fever, cough or shortness of breath.
Loss of smell and taste
In mild to moderate cases of coronavirus, a loss of smell and taste is emerging as one of the most unusual early signs of COVID-19.
"Anosmia, in particular, has been seen in patients ultimately testing positive for the coronavirus with no other symptoms," according to the American Academy of Otolaryngology-Head and Neck Surgery.
A recent analysis of milder cases in South Korea found the major presenting symptom in 30% of patients was a loss of smell. In Germany, more than two in three confirmed cases had anosmia.
Is there anything you can do at home to test to see if you're suffering a loss of smell? The answer is yes, by using the "jellybean test" to tell if odors flow from the back of your mouth up through your nasal pharynx and into your nasal cavity. if you can pick out distinct flavors such as oranges and lemons, your sense of smell is functioning fine.
Fatigue
For some people, extreme fatigue can be an early sign of the novel coronavirus. The WHO report found nearly 40% of the nearly 6,000 people with laboratory confirmed cases experienced fatigue.
Fatigue may continue long after the virus is gone. Anecdotal reports from people who have recovered from COVID-19 say exhaustion and lack of energy continue well past the standard recovery period of a few weeks.
Headache, sore throat, congestion
The WHO report also found nearly 14% of the almost 6,000 cases of COVID-19 in China had symptoms of headache and sore throat, while almost 5% had nasal congestion.
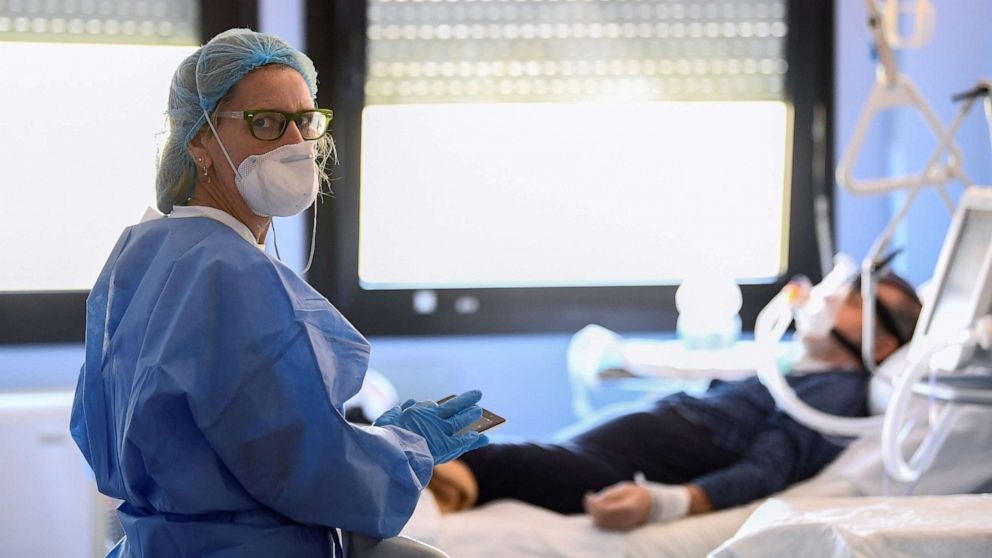 |
| Call doctors if you have symptoms (Photo: ABC News) |
So what should you do?
| Talking to CNN, experts advise anyone with mild to moderate symptoms similar to cold and flu to stay home and try to manage them with rest, hydration and the use of fever-reducing medications. That advice does not apply if you are over age 60, since immune systems weaken as we age or if you are pregnant. Anyone with concerns about coronavirus should call their healthcare provider, according to the CDC. |
It's unclear whether pregnant women have a greater chance of getting severely ill from coronavirus, but the CDC has said that women experience changes in their bodies during pregnancy that may increase their risk of some infections.
"Older patients and individuals who have underlying medical conditions or are immunocompromised should contact their physician early in the course of even mild illness," the CDC advises.
"People under 60 with underlying illnesses, with diabetes, heart disease, immunocompromised or have any kind of lung disease previously, those people are more vulnerable despite their younger age," Schaffner said.
A history of travel to an area where the novel coronavirus is widespread (and those parts of the world, including the US, are going up each day) is obviously another key factor in deciding if your symptoms may be COVID-19 or not.
How to be evaluated
If you have no symptoms, please don't ask for testing or add to backlog of calls at testing centers, clinics, hospitals and the like, experts say.
"We do not test people with no symptoms because it's a resource issue," Schaffner said about the assessment center at Vanderbilt. "However, we are emphasizing that people who have this small cluster of important symptoms -- fever and anything related to the lower respiratory tract such as cough and difficulty breathing -- reach out to be evaluated."
If you do have those three signs, where should you go?
"If you have insurance and you're looking for a provider or someone to call or connect with, there's always a number on the back of your insurance card; or if you go online, there is information for patients," Harris said.
"If you don't have insurance, you can start with the state health department or the local community health centers, those are officially known as federally qualified health centers," Harris advised, adding that some states have a 1-800 hotline number to call.
"If there is a testing and assessment center near you, you can go there directly," Schaffer said. "It's always good to notify them that you're coming. Otherwise, you need to call your healthcare provider and they will direct you what to do."
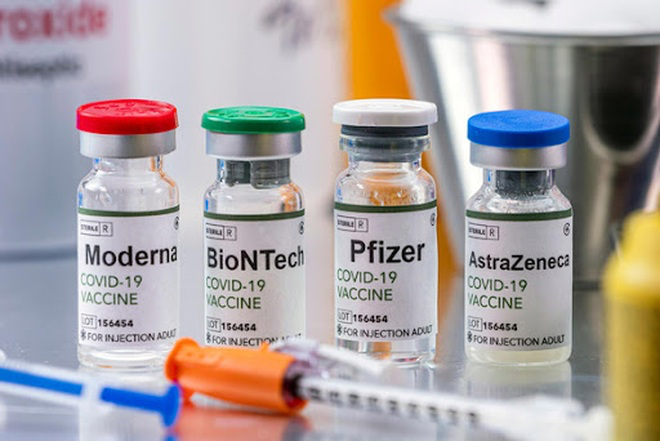
 | Top coronavirus drugs and vaccines in development Coronavirus drugs update: Here are five major coronavirus vaccines and drugs being developed for the treatment of Wuhan coronavirus. coronavirus medicine; corona virus cure; coronavirus ... |
 | Latest treatments and drugs for Coronavieus (COVID-19) Latest Treatments and drugs for Coronavieus (COVID-19): Take a look at several of the latest treatments that doctors hope will help fight COVID-19, the disease caused ... |
 | Military Region 7 presents COVID-19 medical equipment to Cambodian army The High Command of Military Region 7 of the Vietnam People’s Army (VPA) on April 7 handed over medical supplies and equipment to some units ... |
In topics
Recommended
 Handbook
Handbook
Vietnam Moves Up 8 Places In World Happiness Index
 Handbook
Handbook
Travelling Vietnam Through French Artist's Children Book
 Multimedia
Multimedia
Vietnamese Turmeric Fish among Best Asian Dishes: TasteAtlas
 Handbook
Handbook
From Lost to Found: German Tourist Thanks Vietnamese Police for Returning His Bag
Popular article
 Handbook
Handbook
Prediction and Resolution for the Disasters of Humanity
 Handbook
Handbook
16 French Films To Be Shown For Free During Tet Holiday In Vietnam
 Handbook
Handbook
Unique Cultural and Religious Activities to Welcome Year of the Snake
 Handbook
Handbook